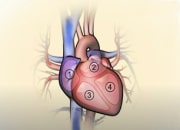
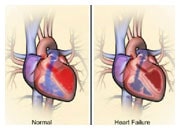
Sleep apnoea and heart failure: the connection explained
The term apnoea means that a person stops breathing for a short period. Patients with heart failure often experience sleep disturbances at night which may include apnoea and episodes of paroxysmal dyspnoea which is typically experienced as sudden shortness of breath while lying down which may lead to awakening and the need to sit or stand up. Abnormal patterns of breathing at night are observed (referred to as sleep-disordered breathing). The most common types of sleep-disordered breathing are central sleep apnoea, obstructive sleep apnoea or a mixed pattern of these two. Careful review of sleep history is essential in making the diagnosis. This includes asking a partner how the patient with heart failure sleeps including a detailed description of the breathing pattern. In particular, asking about episodes of breathing cessation related to snoring is important information.
Central sleep apnoea is a sleep-related disorder in which the patient stops breathing during the night (or breathing diminishes noticeably), typically for 10 to 30 seconds, either intermittently or in cycles. In some cases, it can resemble a rhythmic, waxing and waning pattern of breathing phases including episodes of apnoea (breathing cessation) called Cheyne–Stokes Respiration. In heart failure, this pattern is caused by an abnormal signalling from the brain. Patients with heart failure may have a slower circulation which may impair the ability to rapidly sense changing levels of the blood gases (oxygen and carbon dioxide). This causes the brain to diminish or even stop sending the signals to breathe to the respiratory muscles which are in the chest and diaphragm. This pattern of sleep-disordered breathing is not the same as obstructive sleep apnoea (which can also be present in heart failure) and is caused by an interruption of breathing due to a partial obstruction of normal airflow in the upper airways usually associated with snoring.
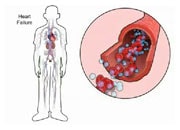
A reduced oxygen level in the blood due to shallow breathing or long pauses of breathing may be deleterious as it can cause patients to wake up frequently throughout the night leading to difficulty falling asleep (insomnia) and tiredness during the day. This oxygen deficit may also trigger surges of stimulation in the sympathetic nervous system, which regulates blood pressure and heart rate, and this activation may have negative effects on the cardiovascular system.
Apnoea and Heart Failure
Patients with heart failure and central sleep apnoea typically report abrupt awakenings accompanied by shortness of breath, difficulties staying asleep, difficulties concentrating, morning headaches and excessive daytime drowsiness. This can cause a patient to fall asleep while at work or even during normal daily activity. Patients also report fatigue and further impairment of exercise tolerance. Anxiety or depression may complicate the symptoms.
Typically, snoring is linked with sleep-disordered breathing, but it more often indicates some degree of upper airflow obstruction (obstructive sleep apnoea). However, snoring and sleep-disordered breathing may also be present in patients without obstruction (central sleep apnoea). Importantly, central sleep apnoea affects not only quality of life but is also associated with a poor prognosis with more frequent hospital admissions, a higher risk of heart rhythm abnormalities and potentially serious complications.
Making the diagnosis of sleep disordered breathing requires detailed evaluation of the patient’s sleep history. Questionnaires are also frequently useful. Overnight polysomnography, during which the breathing pattern is carefully monitored and analysed, may be recommended. Confirmation of a final diagnosis of sleep apnoea sometimes requires evaluation by a specialist physician using advanced equipment to study a patient in a sleep laboratory.
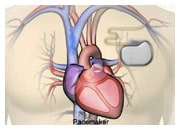
Treatments of central sleep apnoea in patients with heart failure is still controversial. Optimization of the treatment of heart failure is essential, preferably by a heart failure management team, using appropriate medication and specific interventions, such as devices when indicated. Psychotherapy may be recommended for some patients. However, currently there is no specific form of therapy that has been proven to improve outcomes. In the past positive pressure airway masks were sometimes recommended, but recent evidence suggests that they are not useful for patients with heart failure. Other relatively simple alarm devices which respond during periods of apnoea may be useful. In certain patients with severe symptoms, treatment with so-called phrenic nerve stimulation with a device which resembles a pacemaker may be considered. This device is programmed to monitor breathing and sense breathing cessations and long periods of apnoea. The device will then stimulate the diaphragm to restore adequate ventilation and breathing until normal breathing resumes.