Remote monitoring (telemonitoring): tracking heart failure from home
The term “Telemonitoring” encompasses a large variety of innovative approaches designed to improve patient care. It is important to understand that the technical aspects of this technology serve one major objective: enabling a better patient health status with better quality of life.
Telemonitoring uses different types of information technology (IT) to monitor patients at a distance, usually at home. It may involve the transfer of for example blood pressure, heart rate, or body weight through technology. Technologies used are telephone lines, broadband, satellite, or wireless networks.
Also, electrocardiographic signals, oxygen saturation, or the pressure of large arteries within the body can be monitored and transmitted to the care provider. The measurement is done by a specific sensor that defines the type of telemonitoring.
Probably, the simplest yet highly effective way to monitor patients is to contact them regularly by phone. During the phone call, the well-being and physical self-measurements of the patient (e.g. body weight, edema, increasing symptoms) can be checked. If patients can measure their own blood pressure and heart rate this can also be discussed during a phone call. On the call, further educational information can be shared, and potential problems addressed immediately. Using this approach, however, only a limited amount of information can be exchanged and recorded regularly. And only a limited number of patients can be followed in this way due to manpower limitations.
Therefore, new telemonitoring systems have been designed allowing wireless transmission of medically important information. In general, such systems consist of 4 elements:
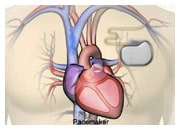
- SENSOR: the device that facilitates measuring the body-related information considered important for making treatment decisions and monitoring the care process. Typical examples are an ECG patch, blood pressure cuff, a wearable device like a watch that tracks activity, or an implanted sensor that relates to a pacemaker or implantable defibrillator.
- LOCAL DATA STORAGE: using a memory device at the patient’s home or sometimes using the memory system in an implanted device. The measurement information can be stored temporarily or long-term.
- CENTRALIZED DATA STORAGE: a secure databank that allows your care provider to interrogate and analyze your measured and transmitted patient information. The data may be stored on the premises of your doctor or at a so-called hosting institution.
- INTEGRATED DIAGNOSTIC TOOL: Often, the measured information is presented graphically over time to your doctor or nurse. Based on this information, medical decisions may be taken. New technology allows sorting and processing the various types of data associated with your care pathway in an intelligible fashion. Underlying software may even provide so-called decision support algorithms. These enable the care team to take care of more patients with high precision and efficiency.
It is essential to understand that the technical solution itself is a tool to improve patients care and is not part of the treatment itself. Rather, the information provided by the sensor needs to be looked at by specifically trained staff, e.g. a heart failure nurse or a physician who then can take appropriate action. A typical action triggered by telemonitoring collected information could be a change in medication or dosage. However, the consequences of these decisions frequently require further actions and supervision, such as re-testing of laboratory values is needed to ensure patient safety.
Please note, that not all telemedical solutions are offered in all countries and telemedical services are not automatically reimbursed by health insurance companies. Ask your doctor for potential options that might be appropriate for your condition.
Quality criteria for data safety and protection of patient privacy include encryption of the transmitted data and dedicated procedures guaranteeing restricted access to your medical data. Of course, participation in any telemonitoring care pathway requires the explicit consent of the patient. The telemedical care provider may ask for additional consent to make use of your data for scientific purposes. Prior to consenting, the patient, and any caretaker, should read the respective patient information sheet carefully.
It is important that before starting any type of remote monitoring plan, patients are fully informed in an understandable language and that an adequate opportunity to ask questions to the health care professional is provided.