Questions to ask your doctor or nurse
It is important to make the most of appointments with your doctor to answer any questions you have about your heart failure treatment. Here we provide a list of general questions and an explanation of why you may find it useful to ask them. You can print these out and take them with you when you next visit your doctor.
MEDICINES
How many tablets should I take and when?
Your doctor, pharmacist or nurse will help you to create your own personal medicine chart to keep a track of when and how often to take your medicines.
Can my medicine(s) cause any side effects?
Asking this question will make sure you know what to expect from taking the medicine, and allow you to prepare yourself for any unwanted side effects, e.g. if dizziness is a side effect of your medication you can prepare by not standing up too quickly and getting out of bed slowly.
Who should I contact if I think I am having a bad reaction to my medicine(s)?
Your doctor will advise you who to contact if you feel unwell after taking your heart failure medicine. You can then make sure you always have the details to hand and share it with family and friends.
What if I miss a tablet?
Your doctor will advise you what to do if you miss one or more doses of your medicine. For most heart failure medicines to work optimally you need to take the correct dose at the correct time. By taking a tablet late, or two tablets at the same time, you may be increasing the amount of medicine in your body to a level which might lead to side effects.
How often do I need to get a new prescription?
Your doctor will prescribe your medicine for a specific amount of time, and will tell you if you need to make another appointment to get a repeat prescription or if you can collect this from your clinic or pharmacy. With most heart failure medicines, it’s important that you take them every day, therefore it’s important to plan ahead to make sure you don’t run out and always remember holidays or planned travel.
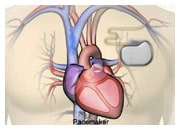
DEVICES
How do I know if I need a device?
Your doctor will evaluate your symptoms and heart function. If your heart beats too slowly, you may need a pacemaker. If you have moderate or serious symptoms of heart failure and evidence of poor, uneven contraction, you may require a CRT. If you have had episodes with serious rhythm disturbance, you may be considered for an ICD.
What are the risks associated with having a device implanted?
Your doctor will be able to tell you the risks involved in having a device implanted. For most patients, the benefits of having a device far outweigh any risks.
Will I need a general or local anaesthetic in order to have the device inserted?
General anaesthetic involves you being put to sleep but with local anaesthetic you will be awake but the part of your body being operated on will be made numb. Your doctor will be able to tell you whether you need a local or a general anaesthetic so that you can be prepared. You may be asked not to eat or drink anything for up to 6 hours before most procedures, including operations under general anaesthetic.
Will I need to stay overnight in hospital when I have my device inserted?
Your doctor will tell you if you need to stay overnight in hospital. This often depends on whether you will be having a general anaesthetic as recovery time will be longer for procedures under general anaesthetic than for a local anaesthetic. You may need to come in to hospital the night before if your device is being inserted early in the morning.
How often will I need to come back to have my device checked?
Your doctor will be able to tell you how often your device needs to be checked. It’s very important to attend these appointments so you should make sure you plan ahead and don’t book a holiday when your device is due to be checked. Your device will need replacing at some point and your doctor will be able to give you an idea of when you should expect this.
Will I be able to travel by plane, drive a car and perform other normal activities?
Following the insertion of your device you should still be able to fly and drive a car and your doctor will be able to advise you on what you should avoid doing. There may be some restrictions on driving after your device has been implanted and this should be discussed. Your doctor or physiotherapist will recommend a programme of gradual physical activity, to make sure that you don’t put too much strain on your body too quickly.
Will I have to take any extra medicines after the device has been inserted?
You may need to take additional medicines, or you may need to change the medicines you were taking before you received the device. Your doctor will tell you what medicines you need to take, how often and for how long. You will then be able to add these into your daily routine and add them to a medicine chart to remind you to take them correctly.
SURGERY AND PROCEDURES
What are the risks associated with this surgery?
Before you have any surgery, your doctor will discuss the procedure and any associated risks. For most patients, the benefits of surgery far outweigh the risks.
Will I have to stay in hospital?
Your doctor will be able to tell you if you need to make arrangements to stay in hospital overnight, you can then plan accordingly.
How long will the surgery/procedure take?
You doctor will be able to give you an idea of how long you the procedure will take and how long you will be in hospital so you can plan accordingly.
Will I feel anything?
Your doctor will inform you whether you will need to have a general or local anaesthetic during the procedure. If it’s a general anaesthetic, you will be put to sleep and you will not be aware of the surgery/procedure taking place. If you are having a local anaesthetic, you will be awake during the procedure, but you shouldn’t be able to feel the operation as the area being operated on will be numb.
Will I have to take any extra medicines following the procedure?
You may need to take medicines after your surgery that are different from those you were taking before the procedure. You could take along the questions on the medicines list so that after your procedure you can check how much to take, how often, and if there are any associated side effects.
How long before I start to feel better?
Your doctor may be able to give you an idea of how long it will take to recover from your operation. While it may not take too long to recover from the surgery, it may take a while for you to notice the benefits of the surgery on your heart failure symptoms.
Will I have to make any lifestyle changes?
After your surgery, you may not be able to go back to your normal diet and physical activity straight away. Your doctor will be able to advise you on what you can do and what you should try to avoid doing.