Low iron in heart failure: symptoms, tests and treatment
Iron deficiency (ID) is the most widespread nutritional deficiency worldwide. It is highly prevalent in patients with heart failure, regardless of the cause. It is also frequently found in patients without anaemia. ID is particularly common in patients with heart failure who are elderly and frail and who often have several other serious medical conditions such as chronic kidney disease, diabetes, or chronic lung disease.
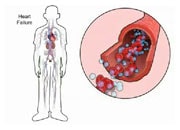
For the majority of people, iron is a nutrient critically needed for optimal formation of red blood cells (erythropoiesis). Iron is an essential part of the haemoglobin molecule which carries oxygen in the blood. Therefore, ID is traditionally linked with anaemia which is a low level of haemoglobin. Anaemia may have many causes but most commonly anaemia is due to reduced production of red blood cells by the bone marrow or chronic blood loss usually from the intestines. Chronic ID may also eventually lead to an iron-deficiency anaemia. Actually, in patients with heart failure, ID alone is approximately 3-times more common than anaemia.
It is important to detect ID by screening patients with a routine blood test. Treatment is recommended regardless of the presence or absence of anaemia. ID itself has numerous clinical unfavourable disadvantages in patients with heart failure. Iron is not only an element of haemoglobin but is present in all cells in the body as a part of mitochondria, which are cellular structures responsible for energy generation. Hence, it is not surprising that iron is particularly needed for tissues with high energy demand, such as the heart and muscles. The symptoms and consequences of ID in patients with heart failure are related to an abnormal functioning of the muscles in the body and the heart itself.
The exact origin of ID in patients with heart failure is not completely understood. In general, it is associated with inadequate dietary iron intake, increased iron losses and an abnormal iron distribution to body compartments where it is not available for use in body metabolism (cellular processes). ID can also be due to poor absorption of iron by the intestines, the use of certain drugs which lower gastric acidity such as drugs commonly used for indigestion and reflux. Certain foods that contain “phytates” such as cereals, grains and beans may reduce iron absorption. Iron loss may occur due to menstrual blood loss or some common gastrointestinal disorders, for example, peptic ulcer or colitis.
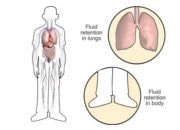
ID in patients with heart failure may result in a worsening of typical symptoms such as shortness of breath, fatigue, impaired exercise capacity and poor quality of life. ID also increases the risk of hospitalisation due to heart failure and may also lead to other serious complications.
Because of potential detrimental effects of ID in patients with heart failure, it is recommended that patients with heart failure should be routinely screened for the presence of ID. The blood tests that are used are called serum ferritin (level of iron in the blood) and transferrin saturation (TSAT) which measures the saturation of the protein that carries iron in the blood. These tests will detect the presence of ID requiring treatment regardless of haemoglobin level. The following definition of ID is recommended for use in patients with heart failure: serum ferritin <100 μg/L, or serum ferritin between 100–299 μg/L and TSAT <20%. Both tests are necessary in that that neither serum ferritin nor TSAT alone are reliable for the assessment of iron status in patients with heart failure. Patients should discuss questions about their iron status with their doctor or nurse.