Implantable Cardioverter Defibrillator (ICDs)
What does it do?
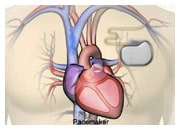
An Implantable Cardioverter Defibrillator (ICD) is a pacemaker-like device that continuously monitors your heart rhythm. If it senses there is a minor problem with the rhythm, it delivers a series of painless electrical impulses to correct the heart rhythm. If this doesn’t work, or a more serious heart rhythm problem is detected, the ICD will deliver a small electrical shock, known as cardioversion . If this doesn’t work, or a very serious problem is detected, the device will deliver a more noticeable shock to the heart, known as defibrillation.
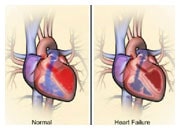
ICDs are generally used in people at high risk of serious rhythm problems in the ventricles (lower chambers) of their heart, as this is the primary cause of sudden cardiac death. In certain patient groups with heart failure, these devices have been shown to prolong survival. Doctors often choose to combine an ICD with a CRT in the same device. In this case, the device is termed a CRT-D.
Where does it go and how is it put in place?
An ICD is usually implanted under local anaesthetic, just below your collarbone with flexible electrode leads (coated wires) coming from it that are positioned in your heart. The procedure usually takes 1-2 hours.
The electrode lead(s) is inserted into a vein at the shoulder or the base of the neck. The cardiologist guides the lead into the correct chamber of the heart, checking its position on an X-ray screen and securing it in position with a stitch at your shoulder. The lead is then connected to the pulse generator and the ICD is fitted into a small ‘pocket’, or space, between the skin and the chest muscle. The device is then tested before the wound is closed.
After the procedure
After your ICD has been fitted, you may feel some pain or discomfort and there may be some bruising at the site of the ICD, but these problems usually disappear in a few days. Most people are able to walk around later the same day and resume normal activities within 2-4 weeks.
The functioning and battery life of your ICD must be checked regularly at a pacemaker clinic. Depending on the device implanted, a Telemonitoring follow-up may be proposed to monitor your device, allowing rapid identification of heart rhythm disturbance and technical dysfunction as well as improving your care and reducing the need for device clinic visits.
Only the device needs to be replaced (not the leads) if the battery runs out. The battery usually lasts between 5 and 7 years before it needs replacing. It’s important that you let any doctors or dentists know that you have an ICD before going for any procedures. Although most medical and dental procedures are not likely to interfere with the functioning of your device, some may require precautionary measures that minimise any interference. ICDs may sometimes be detected by airport security machines, so if you have an ICD you should always inform security personnel; however, the functioning of the device is rarely affected.
Only the device needs to be replaced (not the leads) if the battery runs out. The battery usually lasts between 5 and 7 years before it needs replacing. It’s important that you let any doctors or dentists know that you have an ICD before going for any procedures. Although most medical and dental procedures are not likely to interfere with the functioning of your device, some may require precautionary measures that minimise any interference. ICDs may sometimes be detected by airport security machines, so if you have an ICD you should always inform security personnel; however, the functioning of the device is rarely affected.
There are two types of ICDs:
- Single-chamber ICD
- Dual-chamber ICD