Types of heart failure: what the different terms mean
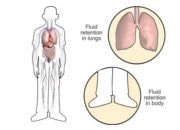
Heart failure may affect different patients very differently – the affected parts of the heart, the resulting symptoms and the time course of heart failure onset can vary widely. For this reason, different medical terms are used to exactly describe the different types of heart failure. It’s very important to define the type and cause of heart failure because it determines treatment. Exact diagnosis may be difficult since symptoms may be very similar, for example, all types of heart failure cause shortness of breath, fatigue and some degree of congestion, usually in the lungs but also in other parts of the body such as the liver, intestines, kidneys and lower limbs.
Acute heart failure develops suddenly and symptoms are initially severe. Acute heart failure may follow a heart attack, which has caused damage to an area of your heart. It may also be caused by a sudden lack of ability by the body to compensate for chronic heart failure. If you develop acute heart failure, it may be severe initially, but may only last for a short period of time and improve rapidly. It usually requires treatment and medication to be administered by injection (intravenously).
Chronic heart failure is very common. Symptoms appear slowly over time and gradually get worse.
If symptoms, such as shortness of breath, get worse within a very short period of time in a patient with chronic heart failure, we call this an episode of acute decompensation. These episodes often need to be treated in hospital and should therefore be avoided. Heartfailurematters.org can help you to avoid hospitalisations.
Please note that heart failure may be caused or worsened by irregular heart rhythm or a fast heartbeat because this impedes proper filling of the ventricles. It’s important to detect such trigger factors in order to treat them and to avoid them in the future.
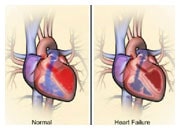
Left-sided heart failure means that the power of the left heart chamber, which pumps blood throughout the body, is reduced; thus, the left chamber must work harder to pump the same amount of blood.
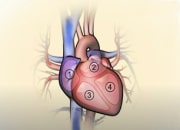
There are two types of left-sided heart failure:
- Systolic failure: The left chamber lacks the force to push enough blood into circulation.
- Diastolic failure: The left chamber fails to relax normally because the muscle has become stiffer and filling is impaired.
The term ejection fraction is used to describe the chambers’ strength and ability to empty with each beat. It can be measured in many ways but usually with echocardiography. If the pumping ability of the main pumping chamber is reduced, it’s often referred to as HFrEF or Heart Failure with reduced Ejection Fraction. If the primary problem is abnormal relaxation during diastole, which impairs filling, the term HFpEF, or Heart Failure with preserved Ejection Fraction is often used. There is often overlap between these conditions with both reduced emptying and filling.
In right-sided heart failure, the right pumping chamber or ventricle, which pumps blood to the lungs, is compromised. This may be due to muscle injury, such as a heart attack localised to the right ventricle, damage to the valves in the right side of the heart or elevated pressure in the lungs.
However, heart failure commonly affects both sides of the heart and is then called biventricular heart failure.